The CDC released the 2019 Antibiotics Resistance Report
 The Centers for Disease Control and Prevention (CDC) released its 2019 report on Antibiotic Resistance Threats in the United States. The report shows that antibiotic-resistant bacteria and fungi cause more than 2.8 million antibiotic-resistant infections, and consequently more than 35,000 people die each year in the US.
The Centers for Disease Control and Prevention (CDC) released its 2019 report on Antibiotic Resistance Threats in the United States. The report shows that antibiotic-resistant bacteria and fungi cause more than 2.8 million antibiotic-resistant infections, and consequently more than 35,000 people die each year in the US.
The 2019 report included, for the first time, the infection and death estimates for healthcare-associated microorganisms. These estimates were calculated using electronic health data from hospitals. Therefore, the original data from 2013 cannot be compared to the data from 2019. The CDC re-calculated the data from 2013 to show the comparisons.
The data in the report indicates that the original data of the 2013 report on antibiotic resistance in the US did underestimate the problem. Data sources not available in the past were used in the 2019 report. As a result, the report shows that there were almost twice as many annual deaths from antibiotic-resistant infections as initially reported in 2013. The 2019 data shows that since 2013, prevention efforts have reduced deaths from antibiotic-resistant diseases by 18% overall and by nearly 30% in hospitals. However, this progress may be challenged by the increasing burden of some infections without continued diligence.
The report categorizes the antibiotic-resistant bacteria and fungi into three categories based on the level of concern to human health: (i) urgent; (ii) serious, and (iii) concerning.
Urgent Threats
Five microorganisms are included in this category. Two of them (drug-resistant Candida auris and carbapenem-resistant Acinetobacter) are new in this report.
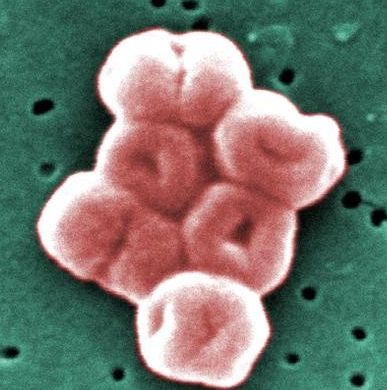
Carbapenem-resistant Acinetobacter causes pneumonia and wound, bloodstream and urinary tract infections. Nearly all these infections happen in patients who recently received care in a healthcare facility. Data for 2017 estimates cases in hospitalized patients at 8,500 and estimated deaths at 700. Infections with this bacterium often arise in health care settings and appear to be resistant to multiple antibiotics.
Drug-resistant Candida auris (C. auris) is an emerging multidrug-resistant yeast. It can cause severe infections and spreads quickly between hospitalized patients and nursing home residents, and kills 1 in 5 infected people. The number of clinical cases in 2018 was estimated at 323.
Drug-resistant Clostridioides difficile can cause life-threatening diarrhea and colitis. According to the report these bacteria often infect people who are currently taking or have recently stopped taking antibiotics. Infections per year: 223,900; Deaths per year: 12,800.
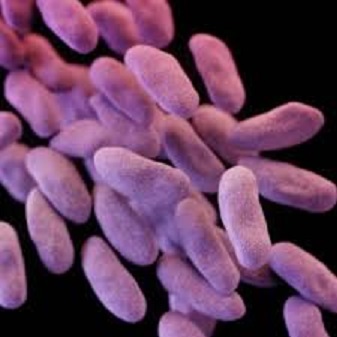
Carbapenem-resistant Enterobacteriaceae (CRE) is a major concern for patients in healthcare facilities. Some Enterobacteriaceae are resistant to nearly all antibiotics, leaving more toxic or less effective treatment options. Estimated cases in hospitalized: 13,100; Estimated deaths: 1,100.
Drug-resistant Neisseria gonorrhoeae causes the sexually transmitted disease gonorrhea that can result in life-threatening ectopic pregnancy and infertility and can increase the risk of getting and transferring HIV. Estimated drug-resistant infections per year: 550,000, which is twice as many as reported in 2013.
Recently there have been fewer infections reported from the urgent threat category carbapenem-resistant Enterobacteriaceae (CRE) that have remained stable. This is an accomplishment after the quick and broadly spread of this organism across the United States in the early 2000s.
Serious Threats
This group includes 11 microorganisms, some are listed below:
ESBL-producing Enterobacteriaceae (Extended-spectrum β-lactamase) can spread rapidly and cause or complicate infections in healthy people. ESBL stands for extended-spectrum beta-lactamase. ESBLs are resistant to penicillins and cephalosporins. ESLB is one of the leading causes of death from resistant germs. They make urinary tract infections harder to treat, especially in women, and could undo the progress made in hospitals if allowed to spread there. Estimated cases in hospitalized patients: 197,400; estimated deaths: 9,100.
Drug-resistant Campylobacter usually causes diarrhea (often bloody), fever, and abdominal cramps, and can spread from animals to people through contaminated food, especially raw or undercooked chicken. Drug-resistance infections per year: 448,400; estimated deaths per year: 70.
Vancomycin-resistant Enterococcus (VRE) Enterococci can cause serious infections for patients in healthcare settings, including bloodstream, surgical site, and urinary tract infections. Estimated cases in hospitalized patients: 54,500; estimated deaths: 5,400.
Methicillin-resistant Staphylococcus aureus (MRSA) are common bacteria that spread in healthcare facilities and the community. MRSA can cause difficult-to-treat staph infections because of its resistance to some antibiotics. Estimated cases in hospitalized patients: 323,700 ; Estimated deaths in 2017: 10,600.
Drug-resistant Streptococcus pneumoniae causes pneumococcal disease, which can range from ear and sinus infections to pneumonia and bloodstream infections. Erythromycin-resistant group A Streptococcus causing Invasive infections have quadrupled since the 2013 report. If resistance continues to grow, infections and deaths could rise. Estimated infections: 900,000; estimated deaths: 3,600.
Final Thoughts

Deaths from antibiotic-resistant infections in hospitals went down 28% from 2012 to 2017. However, microorganisms continue to spread and develop new types of resistance, and progress is slowed by infections that are on the rise. More action is needed to address antibiotic resistance.
Antibiotic-resistant microorganisms are often found in healthcare, including CRE and methicillin-resistant Staphylococcus aureus (MRSA), which caused more than 85% of the total deaths calculated in the report.
Despite the progress made, the threat from microorganisms is increasing over time. The world is seeing a rapid emergence of resistance in microorganisms making the current antibiotics less effective. The evolvement of resistance can be attributed to overuse of antibiotics, and reduced economic incentives to develop new antibiotics (Since 1990, 78% of major drug companies have scaled back or cut antibiotic research). Antibiotics resistance spreads easily around the world through people, animals, and goods.
